The CMS Hospital Price Transparency Rule took effect almost a year ago, but, as we’ve noted in past blog posts, most hospitals in the US have yet to publish their price transparency files. We decided to look at compliance by state to see whether we could learn anything by identifying states whose hospitals have the highest and lowest average compliance rates. Here’s a look at what we found.
Hospital Price Transparency Compliance by State
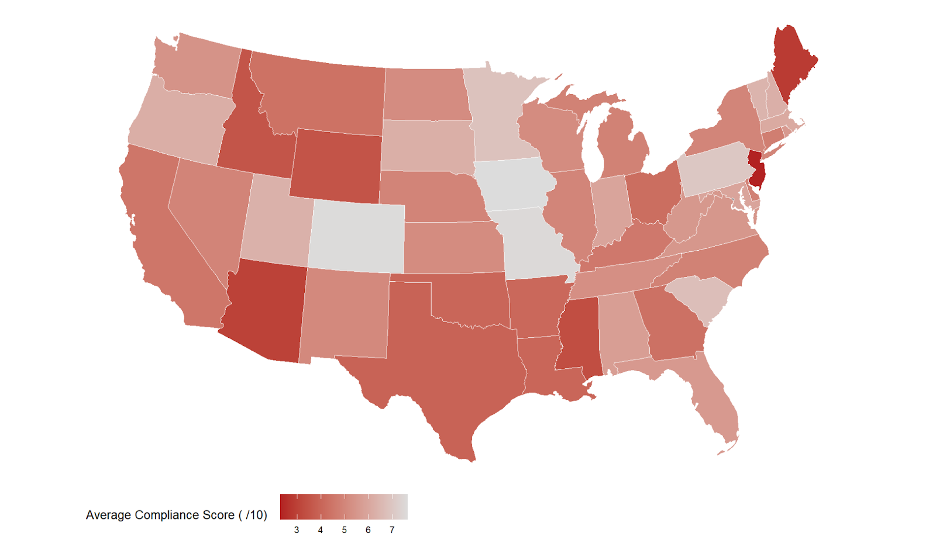
Figure 1: Healthcare Data Analytics heatmap of overall hospital compliance by state
For the heatmap in Figure 1, we colored each state in the continental US based on the average compliance score of its hospitals.* Lighter shades correspond to higher average compliance scores; darker red shades to lower average compliance scores.
According to our analysis, Colorado and Minnesota were among the states with the highest average compliance scores, while Arizona and Wyoming were among the lowest.
These findings didn’t surprise us: both Colorado and Minnesota have state-level price transparency laws that took effect before the CMS’s guidelines did at the start of the year, suggesting that compliance rates may improve with time.
Both Arizona and Wyoming, on the other hand, are among the states with the weakest state-level price transparency protections (see Figure 2).
But state-level laws don’t account for everything in this map. New Jersey, for example, passed a price transparency law in 2018 but still had one of the lowest average compliance ratings state-wide.
So what else is at play here? For one thing, the definition of “transparency.”
Definitions of Transparency Matter
Our map measures compliance with CMS’s law. Another interesting map to consider is the one produced by the Pioneer Institute in 2020 (and reproduced in Figure 2).
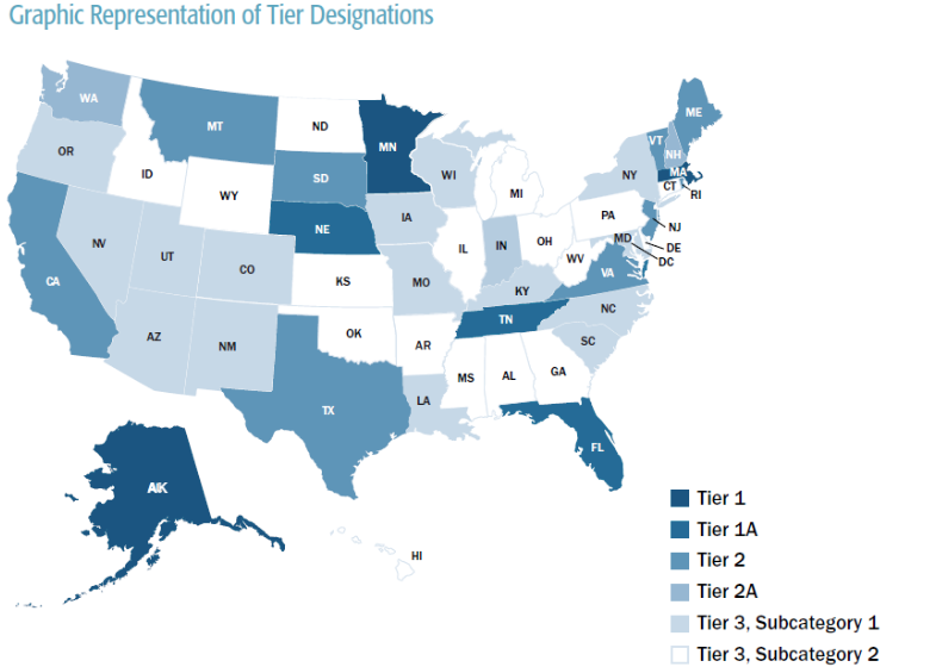
Figure 2: Pioneer Institute map of state price transparency laws across the US (source)
This map evaluates the strength of state-level healthcare price transparency laws, but its criteria don’t correspond to what will make a state compliant with CMS regulations (which, at the time this map was published, were in draft form).
Key to the Pioneer Institute’s evaluation was whether a state’s law allowed individual healthcare consumers to get individualized price estimates for non-emergent care. The “Tier 3” states are ones with no requirement for individualized estimates, though about half have, according to the study, a more general private or government-run price estimator tool.
This may sound academic, but as we seek solutions for greater price transparency, we need to remember that the way we define “transparency” matters, both for…
- Our evaluation of which hospitals and states are doing well (and therefore which need to do more).
- Patient outcomes. Transparency offers a lot of value to a lot of parties. It’s important not to lose sight of the fact that, ultimately, the end game is to make people healthier.
That brings us to our next point.
Compliance Is the Start of the Journey for Consumer-Friendliness
The CMS rule currently requires hospitals to publish pricing data in both a machine-readable and a consumer-friendly format. Even if every hospital in the US were 100 percent compliant, though, the results wouldn’t be all that consumer-friendly.
Without some third-party comparison tool, consumers would still be required to visit the website of every individual hospital where they were considering getting treatment, figure out where that facility’s prices were published, and somehow track those prices to compare them and make a decision.
That’s a far cry from the ease with which consumers can, say, comparison shop for hotels or airfare.
One thing we’re particularly excited about at HDA is the way access to aggregated, standardized data will enable the creation of price comparison tools that can truly transform the experience of shopping for care and choosing providers.
Functional Transparency Will Require a Multi-Pronged Effort
Considering state-level compliance, especially alongside a look at state-level transparency laws, offers further support for the findings of this Robert Wood Johnson Foundation study on price transparency.
Among the report’s recommendations for improving compliance: bring more parties, including states, into enforcement efforts. The existence of so many state-level laws suggests that states could, indeed, have valuable infrastructure in place that could help power enforcement.
States may also be able to pass legislation more quickly than the federal government incentivizing employers and payers to choose hospitals that are compliant with the CMS rule.
Or maybe “enforcement” will emerge more as a market force, with the creation of consumer-facing price aggregation tools that can pull data from – and drive customers to – only those hospitals that have their prices published compliantly.
Let Us Be Part of Your Journey Toward Price Transparency
At HDA, we’re committed to improving price transparency in US healthcare, which we believe will drive innovation and better health outcomes.
Today, we’ve found that we can add value to hospitals at many stages of the journey to price transparency: as consultants guiding them through the process of publishing data, as data analysts helping them identify errors and inconsistencies in their data sets, and as vendors who can provide access to data and analytics tools to see how their prices compare with competitors.
We can also provide data access to other participants in the system: health systems, self-insured corporate plans, and financial firms that could benefit from this competitive data.
Wherever your organization is today, we’d love to be part of your journey toward price transparency. Get in touch to find out how we might do that.
*Note: This data set is current as of November 30, 2021. It is an average compliance score (out of 10 possible points) for all hospitals in the state, including those that have not published any pricing data.
